Senile Purpura: Senile Purpura is a benign bruising condition that affects older adults. It’s also known as actinic Purpura. Our skin and blood vessels become more delicate as we get older, making even minor traumas more likely to cause bruises. This is distinct from problems that result in easy bruising as a result of bleeding issues.
 What is Selina Purpura?
What is Selina Purpura?
![]() Selina purpura is the dark purple scars on the skin, also known as “Actinic purpura” and “Solar purpura,” which were initially discovered by Bateman in 1818. He concluded that these scars were caused by blood extravasation into the dermal tissue.
Selina purpura is the dark purple scars on the skin, also known as “Actinic purpura” and “Solar purpura,” which were initially discovered by Bateman in 1818. He concluded that these scars were caused by blood extravasation into the dermal tissue.
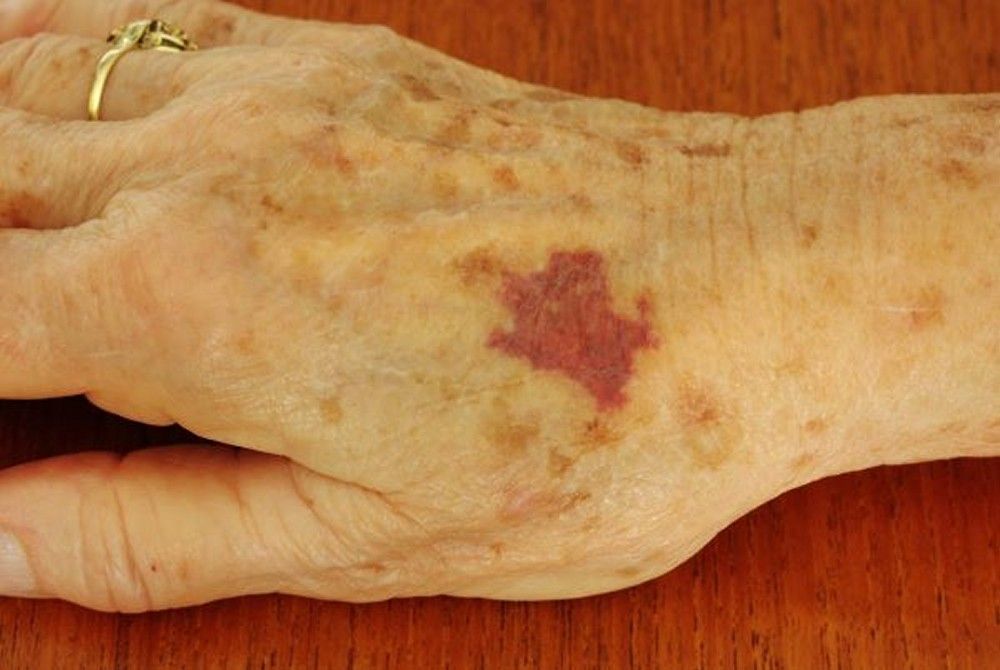
![]() A distinguishing feature of patients with this disorder is the development of persistent dark purple ecchymoses on the extensor surfaces of their hands and forearms. It is unusual for senile Purpura to grow into brown patches like other ecchymosis, although some brown pigmentation may remain for weeks to months or even be permanent.
A distinguishing feature of patients with this disorder is the development of persistent dark purple ecchymoses on the extensor surfaces of their hands and forearms. It is unusual for senile Purpura to grow into brown patches like other ecchymosis, although some brown pigmentation may remain for weeks to months or even be permanent.
![]() The disease is aesthetically unappealing, has no negative health effects. Senile purpura victims are often embarrassed by their purple blotches and try to wear concealing apparel in an effort to avoid being seen.
The disease is aesthetically unappealing, has no negative health effects. Senile purpura victims are often embarrassed by their purple blotches and try to wear concealing apparel in an effort to avoid being seen.
Symptoms
![]() Despite what some people believe, the elderly don’t suddenly wake up covered in reddish-purple patches. Senile purpura symptoms might emerge before bruising in some people. Some of these symptoms are listed below.
Despite what some people believe, the elderly don’t suddenly wake up covered in reddish-purple patches. Senile purpura symptoms might emerge before bruising in some people. Some of these symptoms are listed below.
-
Adjacent skin is often thin, not very elastic.
-
Some of these symptoms are listed below.
-
Skin that is too thin
-
The skin rips readily.
-
Irregular-shaped lesions of one to four centimeters in diameter and dark in color emerge. Usually, they appear on the hands and forearms. However, they may also occur on the face or neck.
-
Bruises appear with or without minor trauma
-
Bruising typically fades after three weeks.
-
Yellowish or brown stains appear where purple bruises once were
-
Bruises recur as a symptom of the disease.
![]() Senile Purpura doesn’t change color like a normal bruise, which is one of the differences between the two. Senile purpura-induced bruises don’t fade; they stay purple the whole time.
Senile Purpura doesn’t change color like a normal bruise, which is one of the differences between the two. Senile purpura-induced bruises don’t fade; they stay purple the whole time.
![]() A yellow or brown stain may temporarily replace the purple bruise in some situations, but the yellowish stain is permanent in others. Senile Purpura may be difficult for some individuals to deal with. For minor wounds, people try to cover them up with make-up to hide them.
A yellow or brown stain may temporarily replace the purple bruise in some situations, but the yellowish stain is permanent in others. Senile Purpura may be difficult for some individuals to deal with. For minor wounds, people try to cover them up with make-up to hide them.
Prevalence of Senile Purpura
![]() Seniors are the most likely to suffer from senile Purpura, affecting around 11.9% of those over 50. Individuals with higher levels of sun exposure are also more likely to be affected. Only two percent of persons over 60 suffer from senile Purpura, which rises to 25 percent for those over the age of 90.
Seniors are the most likely to suffer from senile Purpura, affecting around 11.9% of those over 50. Individuals with higher levels of sun exposure are also more likely to be affected. Only two percent of persons over 60 suffer from senile Purpura, which rises to 25 percent for those over the age of 90.
Causes and Risk Factors
![]() Senile Purpura’s most prevalent cause is aging skin. The skin thins and becomes more vulnerable as we get older. The connective tissues that keep the blood vessels in place deteriorate with repeated exposure to ultraviolet (UV) radiation. Because of this vulnerability, the blood vessels become more brittle, allowing red blood cells to seep into the deeper layers of the skin, resulting in the Purpura.
Senile Purpura’s most prevalent cause is aging skin. The skin thins and becomes more vulnerable as we get older. The connective tissues that keep the blood vessels in place deteriorate with repeated exposure to ultraviolet (UV) radiation. Because of this vulnerability, the blood vessels become more brittle, allowing red blood cells to seep into the deeper layers of the skin, resulting in the Purpura.
![]() Senile Purpura is more common among the elderly; however, natural aging is not the leading cause. If a person spends a lot of time in the sun, the skin’s aging process may speed up. Those who use blood thinners or steroids on a daily basis may be more susceptible to Purpura than the average person. NSAIDs, which are non-steroidal anti-inflammatory medicines, may potentially be a factor.
Senile Purpura is more common among the elderly; however, natural aging is not the leading cause. If a person spends a lot of time in the sun, the skin’s aging process may speed up. Those who use blood thinners or steroids on a daily basis may be more susceptible to Purpura than the average person. NSAIDs, which are non-steroidal anti-inflammatory medicines, may potentially be a factor.
![]() Purpura may be caused by various vascular illnesses, including lupus, rheumatoid arthritis, and Sjogren’s syndrome. Some malignancies, such as lymphoma and leukemia, may also cause purpuras as a side effect. Severe lack of platelets in the blood may lead to bleeding and bruises in the dermis, similar to senile Purpura.
Purpura may be caused by various vascular illnesses, including lupus, rheumatoid arthritis, and Sjogren’s syndrome. Some malignancies, such as lymphoma and leukemia, may also cause purpuras as a side effect. Severe lack of platelets in the blood may lead to bleeding and bruises in the dermis, similar to senile Purpura.
The following are some possibilities:
-
Scurvy
-
Fragile blood vessels
-
Chronic stasis
-
Variations in blood pressure during childbirth
-
Chronic stress
-
Injuries and trauma
-
Systematic disease
-
Anticoagulant therapy
-
Diabetes
-
TORCH infections.
Senile Purpura may potentially be a symptom of skin and bone collagen loss. The loss of collagen in the skin may indicate a comparable decline in bone health to that seen in the skin.
Diagnosis
![]() During the diagnosis of senile Purpura, the doctor will examine the patient’s hands, legs, neck, face, and underarms. The presence of any bruising or thinning of the skin will be documented. Beam’s arms are also expected to be tested. Capillary walls are examined in this study. Platelet testing, capillary fragility tests, and hemostasis tests—which screens for blood clotting difficulties and platelet plugs—are possible.
During the diagnosis of senile Purpura, the doctor will examine the patient’s hands, legs, neck, face, and underarms. The presence of any bruising or thinning of the skin will be documented. Beam’s arms are also expected to be tested. Capillary walls are examined in this study. Platelet testing, capillary fragility tests, and hemostasis tests—which screens for blood clotting difficulties and platelet plugs—are possible.
![]() It is common practice to employ the senile purpura differential diagnosis. When two or more illnesses have identical symptoms, it is necessary to distinguish between them. The following is a list of the most common tests used in the diagnosis of senile Purpura.
It is common practice to employ the senile purpura differential diagnosis. When two or more illnesses have identical symptoms, it is necessary to distinguish between them. The following is a list of the most common tests used in the diagnosis of senile Purpura.
-
PT, aPTT with INR—this is a coagulation profile.
-
CBC—complete blood count with a differential count
-
A urine examination is recommended to rule out inflammation of the tiny blood vessels (Henoch-Schonlein purpura).
-
In order to rule out hepatitis, an LFT—liver function test—is required.
-
If you’re concerned about inflammation connected to possible vascular disease, you may use ESR or CRP—erythrocyte sedimentation rate or C-reactive protein.
-
RF—rheumatoid factor
-
RFT—renal functions test
-
Skin and blood samples
![]() Purpura has been associated with rheumatoid arthritis, lupus, and Sjogren’s syndrome. These all are collagen vascular disorders. Purpura may also appear in persons with internal malignancies, such as lymphoma, multiple myeloma, and leukemia.
Purpura has been associated with rheumatoid arthritis, lupus, and Sjogren’s syndrome. These all are collagen vascular disorders. Purpura may also appear in persons with internal malignancies, such as lymphoma, multiple myeloma, and leukemia.
Summary
Senile Purpura is a benign bruising condition that affects older adults. A distinguishing feature of patients with this disorder is the development of persistent dark purple ecchymoses on the extensor surfaces of their hands and forearms. Seniors are the most likely to suffer from senile Purpura. Senile Purpura’s most prevalent cause is aging skin.
Treatment and prevention
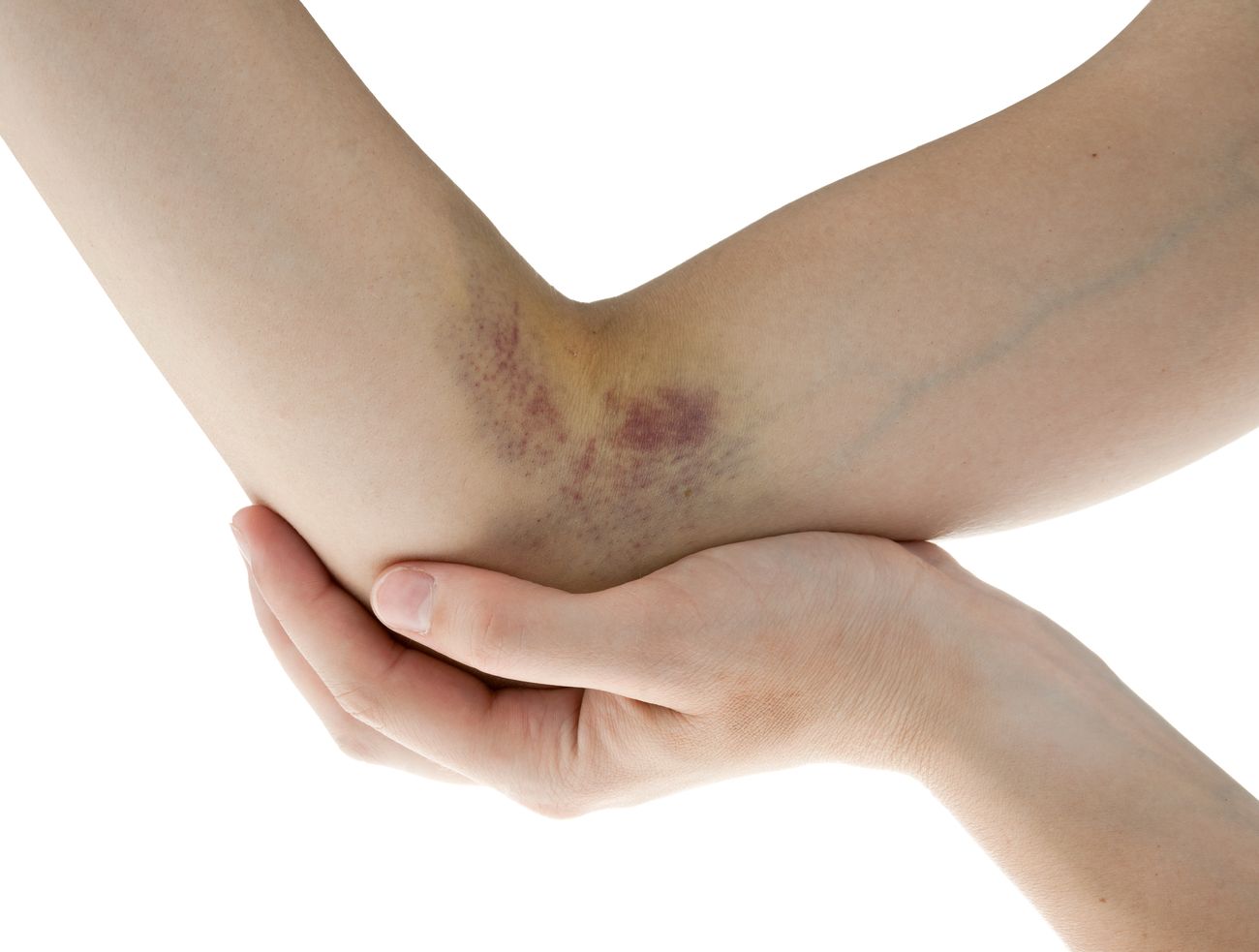
![]() Senile purpura injuries usually are self-healing, and no extra treatment is required. Skin that is very thin might rip, resulting in an open wound at the area of a bruise. Protecting the skin from additional harm is also a good idea. Protect your skin from the sun by wearing long-sleeved clothing and a cap; prevent bumps and bruises as much as possible.
Senile purpura injuries usually are self-healing, and no extra treatment is required. Skin that is very thin might rip, resulting in an open wound at the area of a bruise. Protecting the skin from additional harm is also a good idea. Protect your skin from the sun by wearing long-sleeved clothing and a cap; prevent bumps and bruises as much as possible.
![]() There are several ways to aid those who suffer from senile Purpura to have a better life, including removing the bruises. Researchers in the Journal of Drugs and Dermatology discovered that a verbal medicine meant to treat and prevent senile Purpura was effective in the trial.
There are several ways to aid those who suffer from senile Purpura to have a better life, including removing the bruises. Researchers in the Journal of Drugs and Dermatology discovered that a verbal medicine meant to treat and prevent senile Purpura was effective in the trial.
In patients with senile Purpura, the medication appeared to be safe and beneficial in reducing bruising. When taking medicine, individuals said that their skin seemed to improve in both appearance and quality of life.
![]() For patients who are worried by the appearance of bruises, dermatologists may offer a variety of medications. However, to protect the skin from sun damage, sunscreen can be used by people. Wearing helmets, long sleeves, and sunscreens will not be able to overcome the damage done by the sun, but they may assist in preventing further harm.
For patients who are worried by the appearance of bruises, dermatologists may offer a variety of medications. However, to protect the skin from sun damage, sunscreen can be used by people. Wearing helmets, long sleeves, and sunscreens will not be able to overcome the damage done by the sun, but they may assist in preventing further harm.
For senile Purpura, there is no cone treatment.
 Integrative Treatment
Integrative Treatment
![]() Senile Purpura may be effectively treated with an integrative approach that includes essential nutraceuticals and a single homeopathic medication. Following are the topics that will be covered in this section.
Senile Purpura may be effectively treated with an integrative approach that includes essential nutraceuticals and a single homeopathic medication. Following are the topics that will be covered in this section.
Vitamin C
![]() There are several health benefits of taking vitamin C, including its role in the production of collagen. Scurvy, the most common vitamin C deficient condition, is characterized by bleeding and bruising more often.
There are several health benefits of taking vitamin C, including its role in the production of collagen. Scurvy, the most common vitamin C deficient condition, is characterized by bleeding and bruising more often.
![]() Blood arteries and connective tissue contain collagen, and these symptoms seem to be linked to their deterioration. Maintaining a healthy level of vitamin C seems to be a key factor in preventing Purpura.
Blood arteries and connective tissue contain collagen, and these symptoms seem to be linked to their deterioration. Maintaining a healthy level of vitamin C seems to be a key factor in preventing Purpura.
![]() 94 elderly adults with low vitamin C levels were studied in a double-blind, placebo-controlled study. A decrease in Purpura and petechial hemorrhagesHemorrhage after two months of vitamin C treatment was seen (i.e., a small discrete capillary hemorrhage under the skin).
94 elderly adults with low vitamin C levels were studied in a double-blind, placebo-controlled study. A decrease in Purpura and petechial hemorrhagesHemorrhage after two months of vitamin C treatment was seen (i.e., a small discrete capillary hemorrhage under the skin).
Rutin
![]() There are several health benefits associated with the flavonoid Rutin. 13,14 In solar Purpura, antioxidants play an important role in reducing UV-induced oxidative damage. Additionally, Rutin has been shown to reduce capillary permeability and fragility. Rutin substantially reduced capillary filtration in an 8-month study (P 0.05). Treatment with Rutin also reduced capillary filtration in other studies.
There are several health benefits associated with the flavonoid Rutin. 13,14 In solar Purpura, antioxidants play an important role in reducing UV-induced oxidative damage. Additionally, Rutin has been shown to reduce capillary permeability and fragility. Rutin substantially reduced capillary filtration in an 8-month study (P 0.05). Treatment with Rutin also reduced capillary filtration in other studies.
Citrus bioflavonoids
![]() Diosmin, eriodictyol, hesperidin, neohesperidoside, naringenin, eriocitrin, neodiosmin, rutinoside, chrysoeriol, isorhamnetin, limocitrin, limocitrol, isolimocitrol, and other citrus bioflavonoids have antioxidant properties. Citrus flavonoids containing 0.2 percent eriocitrin and 0.2 percent hesperidin lower oxidative stress in animal models of diabetes for 28 days.
Diosmin, eriodictyol, hesperidin, neohesperidoside, naringenin, eriocitrin, neodiosmin, rutinoside, chrysoeriol, isorhamnetin, limocitrin, limocitrol, isolimocitrol, and other citrus bioflavonoids have antioxidant properties. Citrus flavonoids containing 0.2 percent eriocitrin and 0.2 percent hesperidin lower oxidative stress in animal models of diabetes for 28 days.
Hesperidin
![]() Hesperidin increases venous tone, lowers stasis, restores normal capillary permeability, and promotes lymphatic outflow; hesperidin alone is widely used to treat vascular problems such as hemorrhoids and varicose veins. Reduced free radical production may also be achieved by taking hesperidin supplements. Hesperidin has also been shown to have protective effects on the microvascular endothelium in a randomized, controlled crossover trial.
Hesperidin increases venous tone, lowers stasis, restores normal capillary permeability, and promotes lymphatic outflow; hesperidin alone is widely used to treat vascular problems such as hemorrhoids and varicose veins. Reduced free radical production may also be achieved by taking hesperidin supplements. Hesperidin has also been shown to have protective effects on the microvascular endothelium in a randomized, controlled crossover trial.
Eriocitrin
![]() Animal studies have revealed that eriocitrin, a flavonoid in lemons, may protect against oxidative damage. Eriocitrin has been shown to boost plasma antioxidant activity after ■■■■ Treatment. Additionally, eriocitrin’s antioxidant action has been shown by several studies.
Animal studies have revealed that eriocitrin, a flavonoid in lemons, may protect against oxidative damage. Eriocitrin has been shown to boost plasma antioxidant activity after ■■■■ Treatment. Additionally, eriocitrin’s antioxidant action has been shown by several studies.
Arnica montana
![]() Arnica montana is a popular homeopathic treatment for bruises. In a randomized, double-blind, placebo-controlled clinical experiment, A. Montana was tested on 29 facelift patients to determine its effectiveness in minimizing bruising. These patients had less ecchymosis on postoperative days 1, 5, 7, and 10, and these changes were statistically significant on postoperative days 1 and 7 of the study.
Arnica montana is a popular homeopathic treatment for bruises. In a randomized, double-blind, placebo-controlled clinical experiment, A. Montana was tested on 29 facelift patients to determine its effectiveness in minimizing bruising. These patients had less ecchymosis on postoperative days 1, 5, 7, and 10, and these changes were statistically significant on postoperative days 1 and 7 of the study.
![]() If A. Montana’s capacity to prevent bleeding is linked to its ability to minimize bruising, this might explain its efficacy. Treatment with A. Montana and Bellis perennis was observed to minimize postpartum blood loss compared to placebo in a double-blind, placebo-controlled, randomized clinical study.
If A. Montana’s capacity to prevent bleeding is linked to its ability to minimize bruising, this might explain its efficacy. Treatment with A. Montana and Bellis perennis was observed to minimize postpartum blood loss compared to placebo in a double-blind, placebo-controlled, randomized clinical study.
Combining rutin with vitamin C
![]() As part of an open pilot trial, three patients with persistent, progressive pigmented Purpura (PPP) received verbal Rutin and vitamin C supplements. All three patients had their skin lesions completely cleared at the conclusion of the four-week therapy period.
As part of an open pilot trial, three patients with persistent, progressive pigmented Purpura (PPP) received verbal Rutin and vitamin C supplements. All three patients had their skin lesions completely cleared at the conclusion of the four-week therapy period.
![]() There were no reported side effects. At the conclusion of three months of therapy, all of the patients had no lesions left on their skin. Supplementing with rutin and vitamin C helped another patient with PPP, according to a case study.
There were no reported side effects. At the conclusion of three months of therapy, all of the patients had no lesions left on their skin. Supplementing with rutin and vitamin C helped another patient with PPP, according to a case study.
Combining vitamin C, Rutin, citrus bioflavonoids, hesperidin, eriocitrin, and A. Montana
![]() Supplementation with vitamin C and citrus bioflavonoids, hesperidin, eriocitrin, and A. Montana was tested for six weeks in a randomized, multicenter, placebo-controlled, double-blind research to determine its effectiveness in the Treatment of senile Purpura. Involved in the trial were 70 individuals with senile Purpura; 67 completed it. For six weeks, participants were divided into two groups, one getting a supplement mix and the other a placebo drug.
Supplementation with vitamin C and citrus bioflavonoids, hesperidin, eriocitrin, and A. Montana was tested for six weeks in a randomized, multicenter, placebo-controlled, double-blind research to determine its effectiveness in the Treatment of senile Purpura. Involved in the trial were 70 individuals with senile Purpura; 67 completed it. For six weeks, participants were divided into two groups, one getting a supplement mix and the other a placebo drug.
![]() The number of new purpura lesions in the skin region undergoing clinical evaluation decreased statistically. The supplement blend-treated group exhibited a 50% decrease in purpura lesions at the conclusion of the six-week study.
The number of new purpura lesions in the skin region undergoing clinical evaluation decreased statistically. The supplement blend-treated group exhibited a 50% decrease in purpura lesions at the conclusion of the six-week study.
![]() Patients who received the supplement reported seeing a statistically significant improvement in the look of their skin, which matched the findings of an investigator-led global evaluation. There were no reported side effects from either the patients or the researchers. It shows that the supplement mix reduces skin bruising in people with senile Purpura safely and effectively.
Patients who received the supplement reported seeing a statistically significant improvement in the look of their skin, which matched the findings of an investigator-led global evaluation. There were no reported side effects from either the patients or the researchers. It shows that the supplement mix reduces skin bruising in people with senile Purpura safely and effectively.

 What is the outlook for senile Purpura?
What is the outlook for senile Purpura?
![]() It is not hazardous and fully benign, but the problem will certainly return if no modifications are done. Protecting your skin from the sun’s harmful rays may be done by using sunscreen. Between one and three weeks, most purpuric lesions disappear, although the coloring may remain. The best way to get rid of them is to see a dermatologist.
It is not hazardous and fully benign, but the problem will certainly return if no modifications are done. Protecting your skin from the sun’s harmful rays may be done by using sunscreen. Between one and three weeks, most purpuric lesions disappear, although the coloring may remain. The best way to get rid of them is to see a dermatologist.
 Overview of Senile Purpura
Overview of Senile Purpura
| Causes | Symptoms | Diagnosis | Treatment |
|---|---|---|---|
| Aging skin | Thin skin | capillary fragility tests | Vitamin C intake |
| Exposure to ultra Violet rays | Skin tears easily | CBC | Rutin |
| Blood clotting disorders | Bruises appear with or without minor trauma | liver function test | Citrus bioflavonoids |
| Fragile blood vessels | Irregularly shaped lesions appear | ESR or CRP | Eriocitrin |
 Frequently Asked Questions
Frequently Asked Questions
Here are some frequently asked questions regarding senile Purpura.
Q1. Does senile purpura go away?
It is not hazardous and fully benign, but the problem will likely reoccur if no modifications are done. Protecting your skin from the sun’s harmful rays may be done by using sunscreen. Between one and three weeks, most purpuric lesions disappear, although the coloring may remain.
Q2. What age do you get senile purpura?
Over 10% of those aged over 50 years old have senile Purpura, a rare yet debilitating disease. Males and females alike are susceptible to the condition. Long-term exposure to sunlight, the use of corticosteroids and anticoagulants, as well as chronic UV exposure (blood thinners) are the some risks factors.
Q3. Should I worry about Purpura?
Medical attention should be taken by patients who exhibit any of the following symptoms: Bleeding gums, nosebleeds, or blood in the urine or bowel motions are all symptoms of low platelet count—swollen joints, especially in the knees and ankles.
Q4. Can you get one purpura spot?
On mucosal membranes, such as inside the mouth, spots may occur sometimes. It is common for Purpura to form clusters that are centered in a specific part of the body or cover a significant section of it.
Q5. What is the most common cause of Purpura?
Skin aging is considered to be the primary cause of senile Purpura in the olders. The skin thins and becomes more vulnerable as we get older. Connective tissues that keep blood vessels in place degrade over time as a result of UV exposure.
Q6. Can stress cause purpura?
An uncommon and poorly understood clinical presentation, Purpura (also called Gardner-Diamond syndrome, autoerythrocyte sensitization, or the painful bruising syndrome), causes inexplicable, painful bruises to appear most often in patients’ limbs or faces while they are under stress.
Q7. How do you get rid of blood under the skin?
If you see that a bruise is expanding fast, you should attempt to halt the bleeding under the surface. Make sure to keep the bandage in place until you visit a doctor by covering the area with an elastic bandage, such as an Ace wrap. Alternatively, you might apply 15-minute bursts of direct pressure on the area.
Q8. What should you eat if you bruise easily?
Vitamin K-rich foods may help avoid deficiency and lessen the appearance of bruising, which can occur as a result. Kale, spinach, broccoli, lettuce, soybeans, Brussel sprouts, blueberries, and strawberries are all excellent sources of vitamin K. Adding zinc-rich foods to your diet may help mend and strengthen your tissues.
Q9. What is the difference between Purpura and ecchymosis?
If you have spots or patches that range in diameter from 4 to 10 millimeters, you have Purpura. On the other hand, ecchymosis tends to have a more clearly defined boundary and might seem more like a rash than a bruise. Unlike ecchymosis, Purpura isn’t a result of trauma.
Q10. Is Purpura an emergency?
Disseminated intravascular coagulation (DIC), which may occur in both infective and non-infectious illness states, is a rare, life-threatening condition known as purpura fulminans.
Conclusion
Bateman initially characterized senile Purpura in 1836 as a distinct clinical entity that may be identified by the position and form of the lesions and their natural history, and the patient’s age. It affects both men and women.No systemic illness or recognized nutritional deficit has been linked to this condition. It affects both men and women.
A severe degree of senile degeneration of the skin’s exposed surface has been linked to it, and the lesions are likely the result of slight external stress acting on under-supported skin vessels. Despite the presence of deteriorated collagen fibers in the afflicted locations, no increase in elastic tissue has been identified.
Related Articles
Can you Live Without a Liver
EMSculpt Side Effects
How long does it take for ibuprofen to kick in?
