The liver performs fundamental, life-supporting capacities. While you can’t survive without a liver totally, you can live with just piece of one. Many individuals can work well with simply under portion of their liver. Your liver can likewise develop back to standard size inside only months.
 Would you be able to Live Without a Liver?
Would you be able to Live Without a Liver?
 The numerous jobs of the liver
The numerous jobs of the liver
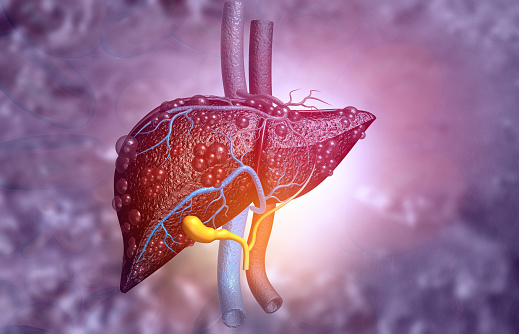
Your liver is a force to be reckoned with, performing more than 500 life-supporting capacities. This 3-pound ■■■■■ — the biggest inside ■■■■■ in the body — is situated in the upper-right piece of your midsection. It does the accompanying:
-
filters poisons from your blood
-
produces stomach related chemicals called bile
-
stores nutrients and minerals
-
regulates chemicals and the resistant reaction
-
helps clump blood
Your liver is the main ■■■■■ in your body that can regrow after pieces of it have been eliminated or harmed. Truth be told, your liver can develop back to its standard in simply an issue of months.
Things being what they are, if the liver recovers, would you be able to live without one for any timeframe? How about we investigate.
 Anyway, would you be able to live without one?
Anyway, would you be able to live without one?
No. The liver is so urgent to presence that while you can live with just piece of a liver, you can’t survive with next to no liver by any stretch of the imagination. Without a liver:
-
your blood will not appropriately clump, causing uncontrolled dying
-
toxins and substance and stomach related results will develop in the blood
-
you’ll have less protections against bacterial and parasitic diseases
-
you can have expanding, including lethal enlarging of the cerebrum
 A liver can fall flat for various reasons.
A liver can fall flat for various reasons.
Intense liver disappointment, likewise called fulminant hepatic disappointment, prompts fast liver crumbling, regularly when the liver was already alive and well. As indicated by research, it’s really uncommon, happening yearly in less than 10 individuals for each million. The most well-known causes are:
 Side effects include:
Side effects include:
The other kind of liver disappointment is known as ongoing liver disappointment. It’s brought about by irritation and scarring that happens over a time of months or a long time. This general liver crumbling is regularly because of things like:
-
alcohol abuse
-
infections, including hepatitis A, B and C
-
liver disease
-
genetic sicknesses, like Wilson’s infection
nonalcoholic greasy liver infection
 Side effects include:
Side effects include:
 Not a capital punishment
Not a capital punishment
However, a faltering liver isn’t a capital punishment. Contingent upon your wellbeing and the soundness of your liver, you might be a possibility for a liver transfer, a medical procedure wherein an ailing liver is eliminated and supplanted with a piece of or a whole solid one from a contributor.
 This implies the liver is taken from a died. individual’s.
This implies the liver is taken from a died. individual’s.
The individual would have marked a giver ■■■■■ card before their passing. The ■■■■■ may likewise be given after death with the assent of the family.The National Institute of Diabetes and Digestive and Kidney DiseasesTrusted Source reports that most gave livers come from expired givers.
 Living giver relocate
Living giver relocate
In this cycle, somebody who is as yet alive — regularly a relative or dear companion — consents to give part of their solid liver.
One studyTrusted Source discovered that of 6,455 liver transfers acted in 2013, just 4 percent were from living benefactors.
Your ■■■ might suggest an orthotopic or heterotopic relocate. In an orthotopic relocate, the ailing liver is completely taken out and supplanted with a sound benefactor liver or section of liver.
In a heterotopic relocate, the harmed liver is left set up and a sound liver or section of liver is placed in. While orthotopic transfers are the most well-known, a heterotopic one might be recommended if:
A specialist might decide on a heterotopic relocate if your liver disappointment is brought about by a hereditary condition that future quality examination might track down a fix or reasonable treatment for.
With your liver flawless, you might have the option to exploit these new advances.
 Is it conceivable to live with part of one?
Is it conceivable to live with part of one?
Despite the fact that you might get just a fractional liver, your PCPs will ensure it’s large enough to fill every vital job.
Truth be told, one transfer specialist at the University of Pittsburgh assesses that you just need 25 to 30 percent of your liver to keep up with typical capacities.
Over the long run, the liver will develop to about its typical size. Specialists aren’t sure precisely how liver recovery happens, yet they do realize that when a liver is carefully decreased in size, a cell reaction is initiated that produces fast regrowth.
 Summary
Summary
The individual would have marked a giver ■■■■■ card before their passing. The ■■■■■ may likewise be given after death with the assent of the family.The National Institute of Diabetes and Digestive and Kidney DiseasesTrusted Source reports that most gave livers come from expired givers.
 Halfway liver expulsion in living benefactor transplantation
Halfway liver expulsion in living benefactor transplantation
Individuals who get a liver from a perished giver will more often than not get relocated with the whole ■■■■■.
The liver may be parted, nonetheless, in case it’s actual huge or it’s being split between a kid and a grown-up.
The individuals who have a living liver gift — which regularly comes from a sound family member or companion who’s coordinated for size and blood classification — get just a piece of the liver.
Certain individuals select this choice since they would rather not hazard getting more debilitated as they look out for a rundown for an ■■■■■ that might possibly come on schedule.
 As indicated by the University of Wisconsin School of Medicine and Public Health:
As indicated by the University of Wisconsin School of Medicine and Public Health:
-
About 40 to 60 percent of the giver liver is taken out and relocated into the beneficiary.
-
Both the beneficiary and the giver will have a sufficient liver to guarantee legitimate working.
-
Regrowth of the liver starts very quickly.
-
Within fourteen days, the liver is approaching its typical size.
-
Total — or close to add up to — regrowth is accomplished inside a year.
In the United States, 14,000 individuals are right now standing by for a relocated liver. Of those, 1,400 will kick the bucket before they at any point get one.
While still not normal, living liver gift is being seen to an ever increasing extent. In 2017, approximately 367 livers were given by living contributors.
A significant advantage of a living liver gift is that the medical procedure can be planned when it’s commonly helpful for the two players. Furthermore, the liver can be given before the beneficiary turns out to be seriously sick. This can help endurance rates.
 To be considered for living liver gift you should:
To be considered for living liver gift you should:
-
be between the ages of 18 and 60
-
have a blood classification that is viable with the beneficiary
-
undergo broad physical and mental testing
-
have a solid weight, since heftiness is a danger factor for greasy liver illness, which harms the liver
-
be able to keep away from ■■■■■■ until recuperated
-
be in great general wellbeing
For more data about being a living liver contributor, contact the American Transplant Foundation. For data on the best way to give your organs after you pass on, visit OrganDonor.gov.
 The focus point
The focus point
The liver performs fundamental, life-supporting capacities. While you can’t survive without a liver totally, you can live with just piece of one.
Many individuals can work well with simply under portion of their liver. Your liver can likewise develop back to standard size inside merely months.
If you or somebody you know has liver infection and needing a transfer, living liver gift might be a choice to consider.
Get our twice week by week health email
To motivate you to practice and eat well, we’ll send you our top wellbeing tips and stories, in addition to must-understand news.
 How does your liver respond?
How does your liver respond?
The liver is an essential ■■■■■ directing the degrees of numerous substances in the body.
The liver is a crucial ■■■■■ directing the degrees of numerous substances in the body. It discharges a substance called bile. The bile helps in diverting the loss from the liver. The blood from the stomach related framework (stomach and gut) goes through the liver.
The liver eliminates poisons from this blood, produces nutrients, and separates the medications taken to innocuous substances. It plays an imperative part in protein, fat, and carb absorption.
The liver weighs around 1.5 kilograms and fills more than 500 crucial roles in the body. Not many of the significant capacities incorporate the accompanying:
-
Bile creation: The liver discharges bile. The bile assists carry with away squandering and separate fats in the small digestive tract during processing.
-
Production of proteins: The liver produces numerous significant proteins, like egg whites and certain proteins, fundamental for resistance and blood coagulating.
-
Formation of cholesterol: The liver structures cholesterol and certain proteins that assist with helping fats through the body.
-
Carbohydrate stockpiling and breakdown: The liver believers overabundance glucose into a steady stockpiling item called glycogen. Glycogen can later be changed over back to glucose when required.
-
Amino corrosive level guideline: The liver manages the blood levels of different amino acids (the structure squares of proteins).
-
Iron digestion: The liver separates hemoglobin to reuse its iron substance. The liver likewise stores iron, which is delivered when the body requires it.
-
Formation of urea: The alkali created during the protein breakdown in the body is profoundly noxious. This is changed over to urea by the liver. Urea is at last discharged in the ■■■.
-
Removal of poisons: The liver aides clear the blood of medications and other poisonous substances.
-
Blood coagulating: The liver delivers a few variables significant in controlling blood thickening.
-
Immunity: The liver produces numerous insusceptible factors and disposes of microorganisms from the blood.
-
Clearance of bilirubin: Bilirubin is delivered because of hemoglobin digestion. The liver aides clear bilirubin through the bile. Bilirubin can be poisonous on the off chance that it amasses in the blood making the skin and eyes become yellow (jaundice). Abundance bilirubin can likewise hurt the cerebrum.
 Would you be able to live without a liver?
Would you be able to live without a liver?
It is absurd to expect to live without a liver. Liver disappointment is a perilous condition that needs dire clinical intercession. If the liver capacity is compromised, like liver disappointment, you can get genuine entanglements, for example,
-
Jaundice (yellowing of the eyes and skin)
-
Tendency to drain
-
Infections
-
Ascites (assortment of liquid in the mid-region)
-
Cerebral edema (extreme liquid in the cerebrum)
-
Kidney disappointment
-
Altered awareness (disarray, bewilderment, tiredness, and even trance state)
-
Fluid and electrolyte unevenness
 Would i be able to give a piece of my liver?
Would i be able to give a piece of my liver?
-
Indeed, you can give a piece of your liver without hurting your wellbeing. The liver is the main ■■■■■ in the body that can recover or develop back if a piece of it is eliminated.
-
At the point when you give a piece of your liver, the part staying in your body becomes back in six to about two months. Additionally, the part relocated will fill in the beneficiary.
-
Inside seven days of the liver gift, the liver capacity gets back to business as usual.
-
Assuming you need to give your liver, you will be expected to finish a passing telephone meet.
-
The meeting is trailed by a total face to face assessment that incorporates blood tests and clinical imaging, like ultrasound, mechanized tomography examine, and attractive reverberation imaging. To be qualified for the liver gift, you ought to:
-
Be matured among 18 and - 55 years. If the liver is to be given to a kid, the benefactor can be as long as 60 years old.
-
Fit enough for medical procedure and recuperation.
-
Free from previous ailments, especially the ones that influence draining or coagulating.
-
Not utilize sporting medications. Albeit smoking doesn’t preclude a contributor, nonetheless, you should stop smoking straightaway before liver gift.
-
Understand the mental and actual dangers implied.
 Liver Regeneration: How does the liver regrow?
Liver Regeneration: How does the liver regrow?
Most gauges say that without a liver, a great many people wouldn’t make due for over a year, and that descending winding wouldn’t be pretty. Be that as it may, something really stands out about the liver, and its almost supernatural regenerative properties.
If you inquire as to whether they will live without an ■■■■■, they’ll likely react with a conclusive NO. What many individuals don’t understand is that you can in reality live without some of your organs.
At times, this is on the grounds that the body contains beyond what one, the capacity can be taken on by one more piece of the body, or methodology exist that can falsely deal with the metabolic burden.
For instance, you can live without a kidney, a stomach, a nerve bladder or a reference section. A few organs can likewise be to some extent eliminated without the result being deadly, like the mind and digestion tracts.
Notwithstanding, what might be said about your liver? What are your odds of getting by without that puzzling ■■■■■?
 Liver: Can’t Live Without It
Liver: Can’t Live Without It
For those of you who don’t have the foggiest idea what’s truly going on with the liver – or even where it is in the body – here’s a fast update. Weighing about 3 beats by and large, the liver is a 4-lobed ■■■■■. It is likewise the biggest glandular ■■■■■ in the body and has some somewhat mind boggling capacities that assistance to keep us alive.
 Where is your liver found?
Where is your liver found?
The liver is situated in the right half of the body in the upper quadrant of the mid-region. It is available underneath the stomach. In view of its size, it likewise goes into the left upper quadrant also. The liver is secured by the lower ribs as it is a sensitive ■■■■■.
 How does the liver respond?
How does the liver respond?
With regards to guaranteeing that our bodies remain poison free, by separating generally 1.5 quarts of blood each moment. With the conceivably risky microorganisms in general and poisons in the blood, without this basic capacity, we wouldn’t keep going extremely long.
-
Past that, the liver is likewise answerable for creating bile, which is essential for processing. Without disposing of poisons and taking in fundamental supplements, we would be not doing so well.
-
As though that wasn’t sufficient, the liver likewise assists with coagulating the blood, in this way forestalling inside dying. At long last, the liver even creates specific proteins that the body needs for appropriate metabolic movement.
-
Obviously, the liver serves some somewhat significant capacities in the body, and keeping in mind that existence without a liver wouldn’t quickly be deadly, it would be a terrible street towards unavoidable passing.
-
Most gauges say that without a liver, a great many people wouldn’t make due for over a year… and that descending twisting wouldn’t be pretty.
-
Shockingly, there are various justifications for why a liver might should be taken out, which makes liver transfers and gifts critical.
-
The most eminent reasons for liver substitution or fractional expulsion incorporate harmless liver masses, hepatocellular carcinoma (prompts essential liver disease), metastatic malignancies of the liver (moved malignant growth cells from other contaminated ■■■■■ frameworks), or cirrhosis of the liver (generally brought about by over the top, long haul ■■■■■■ utilization.
-
These hardships, among a not insignificant rundown of others, can require a fractional or complete evacuation of the liver.
-
While it very well may be not difficult to coordinate givers for different organs that may not be the “great” match, the tissue dismissal rate for livers is higher than in numerous different organs.
-
This implies that undeniably more tests and investigation should be done before a giver liver can be coordinated with a patient needing a substitution. Considering what we just clarified about the fundamental idea of livers, living givers appears to be inconceivable, since that would mean forfeiting their own wellbeing.
-
Nonetheless, there are residing contributors for the individuals who need another liver, which is the place where the most amazing part of the liver becomes an integral factor.
 Liver Regeneration: How does the liver regrow?
Liver Regeneration: How does the liver regrow?
-
While numerous organs have the ability to mend themselves and surprisingly recover little partitions, the liver has a noteworthy capacity to develop back, in any event, when portion of it has been eliminated.
-
Thusly, with regards to halfway liver expulsions, the patient is regularly saved the test of tracking down a giver. The human liver can be chopped down to 25% of its unique size and still capacity appropriately for the human body.
-
More than time, the leftover 75% of the liver will regrow, ultimately leaving the patient with a totally sound liver.
-
The rate at which the liver can develop back is surprising; in the initial two weeks following a medical procedure (halfway expulsion or fractional gift), most of the recovery will happen.
-
This is trailed by a more slow period of regrowth that happens over the course of the following year.
-
In any event, during this period of recovery, the liver can keep on working as would be expected.
-
While most specialists will berate you to lay the ■■■■■■, to stay away from excessive weight on the liver, the wide range of various fundamental elements of the liver won’t be impacted.
-
As referenced over, that is the reason it is feasible to be a living giver of your liver. Assuming an individual requirements a total liver transfer, a direct relation can give a piece of their liver, say 30-40%, and it tends to be set in the body of the patient who needs the transfer.
-
If there is no tissue dismissal, both of you can recuperate ordinarily, and inside a year or thereabouts, you will both have a completely useful liver that is 100% ordinary size.
-
Albeit the tonue is really the quickest mending some portion of the body, because of the rich and consistent stockpile of blood, the liver is extraordinarily capable at recuperating itself, more so than some other significant ■■■■■.
 Your Liver Delivers
Your Liver Delivers
Your liver strives to ensure your wellbeing. It’s a tough, solid ■■■■■. Yet, certain things—like ■■■■■■, drugs, infections, and abundance weight—can harm it.
You may not understand when your liver is battling, on the grounds that liver sickness ordinarily has no manifestations until the issue becomes extreme.
Assist your liver with protecting your wellbeing by staying away from the things that may cause it hurt.
The liver is the biggest ■■■■■ inside your body. It’s with regards to the size of a football, and rests simply under your ribs against the right half of your stomach.
 Non-alcoholic steato-hepatitis.
Non-alcoholic steato-hepatitis.
-
NIH-supported researchers have been looking for less complex ways of estimating the seriousness of greasy liver illness.
-
They’re likewise directing clinical examinations to evaluate potential medicines. There are presently no endorsed meds for greasy liver or its more serious structure called NASH, or non-alcoholic steato-hepatitis.
-
“To treat greasy liver illness, we suggest way of life changes: Weight misfortune for individuals who are overweight, and practice and a solid eating regimen to assist with diminishing fat,” Rotman says.
-
“In numerous patients, simply a 5-8% decrease in body weight will convert into a huge improvement to liver harm.” For individuals with ■■■■■■ related greasy liver, halting ■■■■■■ use can invert or forestall further liver injury.
-
One more typical sort of liver infection—known as viral hepatitis—can be brought about by no less than 5 unique infections, named hepatitis A, B, C, D, and E.
-
These diseases can harm your liver and hold it back from working appropriately.
-
“Aggregately, around 20% of individuals worldwide might be impacted by a hepatitis infection disease,” Liang says. “It’s a significant general medical issue.” The most widely recognized sorts in the United States are hepatitis A, B, and C.
-
Every hepatitis infection causes an alternate type of liver sickness. All the infections can trigger intense, or present moment, hepatitis. Hepatitis B, C, and D can likewise cause ongoing hepatitis, in which the disease endures quite a while, some of the time for what seems like forever.
-
Individuals are regularly presented to hepatitis An and E infections through polluted food or water.
-
The other hepatitis infections regularly go through some sort of break in the skin hindrance, here and there by infusions or by close contact with blood or other body liquids," Liang adds. Hepatitis B, C, and D can spread through sexual contact.
-
Since many contaminated individuals have not many indications, they may not understand they have viral hepatitis. They can spread the disease to others without knowing it.
-
Viral hepatitis is frequently treated with antiviral prescriptions. Hepatitis A, B, and D contaminations can be forestalled by antibodies. Rehearsing great cleanliness—like cleaning up and keeping away from contact with tainted blood—can likewise assist with obstructing the spread of viral hepatitis.
 Summary
Summary
The rate at which the liver can develop back is surprising; in the initial two weeks following a medical procedure (halfway expulsion or fractional gift), most of the recovery will happen. This is trailed by a more slow period of regrowth that happens over the course of the following year.
In any event, during this period of recovery, the liver can keep on working as would be expected. While most specialists will berate you to lay the ■■■■■■, to stay away from excessive weight on the liver, the wide range of various fundamental elements of the liver won’t be impacted
 Some Important Questions Are Discuss Below
Some Important Questions Are Discuss Below
 Frequently Asked Questions (FAQS)
Frequently Asked Questions (FAQS)
 How long can an individual live without liver?
How long can an individual live without liver?
Your liver can continue to work regardless of whether piece of it is harmed or taken out. Yet, if it begins to close down totally—a condition known as liver disappointment—you can make due for just a day or 2 except if you seek crisis treatment.
 Can a liver develop back?
Can a liver develop back?
The liver is the main ■■■■■ in the body that can supplant lost or harmed tissue (recover). The giver’s liver will before long develop back to typical size after a medical procedure. The part that you get as another liver will likewise develop to typical size in half a month
 Do we have 2 livers?
Do we have 2 livers?
The liver has two huge segments, called the right and the left flap. The gallbladder sits under the liver, alongside parts of the pancreas and digestion tracts. The liver and these organs cooperate to process, assimilate, and process food.
 Would you be able to give a liver and live?
Would you be able to give a liver and live?
Living Donor Liver Transplant
Living gift is conceivable on the grounds that the liver is simply the main ■■■■■ that can recover. A grown-up might have the option to give a part of their liver to a youngster or another grown-up.
 Would i be able to give my liver to my father?
Would i be able to give my liver to my father?
Giving your liver is generally something that occurs after you kick the bucket, however it is additionally conceivable to give the endowment of living liver gift. In case you are fit and indeed, it very well might be viewed as conceivable to eliminate section (a flap) of your liver for transplantation to another person
 Conclusion
Conclusion
NIH upholds enormous examination networks the nation over to get familiar with liver sickness. For example, groups of researchers cross country have united to contemplate uncommon and frequently dangerous liver problems that strike babies and more established kids.
“Examination networks are significant in light of the fact that no single clinical focus has enough patients with uncommon sicknesses to do a thorough report or test new therapies,” says Dr. Edward Doo, a liver illness master at NIH. “With this enormous pediatric organization, we can join the endeavors and skill of numerous clinical focuses that work in uncommon youth liver illnesses.”
 Related Articles
Related Articles
You may also like
-
Beauty - How To Discuss
-
https://howtodiscuss.com/t/ideal-weight-for-50-year-old-woman/69347/3