Glomus tumors, also known as paragangliomas, are benign tumors that grow slowly in the carotid arteries (the major blood vessels in your neck), the middle ear, or the area behind the middle ear (jugular bulb). Glomus tumors are usually benign, but they can cause substantial damage to surrounding tissues when they expand.
Glomus Tumor
A Glomus tumor is an uncommon benign soft tissue tumor that arises from the glomus body and presents in the second to fourth decade of life. It accounts for 1-5 per cent of all upper extremity soft tissue tumors.
A glomus body is a component of the skin’s dermis layer that helps regulate temperature. The glomus body is an arterio-venous shunt encased in a connective tissue capsule that is seen in greater abundance in the fingers and toes.
During freezing conditions, the glomus body shunts blood away from the skin surface, avoiding heat loss, and in warm weather, it causes maximum heat flow to the skin.
Glomus tumors appear as painful, blue-red blanch able papules or nodules in the deep dermis or subcutaneous fat, most typically on the fingers and toes and under the nail plate, and are less than 2cm in diameter.
Glomus cells, vascular, and smooth muscle cells make up these structures. These tumors cause significant paroxysmal pain and suffering in the patient when exposed to cold temperatures or pressure fluctuations.
The Love test and the Hildreth sign are two valuable findings for detecting glomus tumors, particularly those under the nails. The Love test entails applying pressure to the suspicious location with a pencil tip or pinhead, eliciting acute pain.
When employing a tourniquet to create transitory ischemia, the Hildreth sign reduces pain and tenderness using the love test. The cause of glomus cell proliferation in glomus tumors is unknown, but there have been ideas that isolated subungual glomus tumors are caused by trauma.
Recurrence is more common in glomus tumors that are skin-colored or situated in the nail matrix. Complete surgical excision is the therapy of choice for symptomatic solitary glomus tumors to reduce the risk of pain recurrence.
Although laser and sclerotherapy have been reported to be beneficial in some cases with single glomus tumors, total excision is the best option.
Preoperative imaging with color Doppler ultrasonography and magnetic resonance imaging for subungual tumors offers information on tumor size, shape, and specific anatomic position. Total nail avulsion and excision are used to treat them.
Excision may be more challenging in cases where there are many glomus tumors due to the significant number of lesions. As a result, multiple studies have shown that argon, carbon dioxide, or Nd: YAG laser therapy, as well as sclerotherapy using hypertonic saline or sodium tetradecyl sulphate, is a better therapeutic option.
The signs and symptoms of glomus tumors:
-
The symptoms of a paraganglioma vary depending on where the tumor is placed.
-
Carotid body tumors (tumors of the carotid arteries) can cause:
-
A swelling in the neck
-
Hoarseness
-
Having difficulty swallowing
-
A tumor of the jugular bulb (glomus jugulare tumor) can cause the following symptoms:
-
One ear is bleeding.
-
Having trouble swallowing
-
Loss of hearing
-
Shoulder sag
The following symptoms can be caused by a tumor in the middle ear (glomus tympanicum tumor):
-
One ear is bleeding.
-
Loss of hearing
-
One ear pulsing or ringing
-
A tumor in the neck (glomus vagal tumor) might cause the following symptoms:
-
Facial numbness or paralysis in a portion of the face (facial palsy)
-
A swelling in the neck
-
The body’s norepinephrine, or stress hormone, levels are sometimes affected by tumors. If this occurs, the following symptoms may occur:
-
Anxiety
-
Headaches
-
Hypertension (high blood pressure)
Glomus Jugulare Tumors: Causes
A glomus jugulare tumor has no recognized cause. In the vast majority of instances, no identified risk factors exist. Glomus cancers have been linked to variations (mutations) in a gene that produces the succinate dehydrogenase enzyme (SDHD).
Pain, soreness, and cold sensitivity are common symptoms of glomus tumors. A case of a characteristic glomus tumor in a young woman was diagnosed and surgically managed successfully.
Medical history and MRI data were used to make the clinical diagnosis. The lesion was excised using a dorsolateral subungual technique, which resulted in total symptom relief. The lesion was determined to be a glomus tumor by histology.
Glomus tumors are a type of subungual lesion that causes pain. Following modest injuries, they cause throbbing or lancinating local discomfort, cold sensitivity, and acute pain. Although histology confirms the diagnosis, the clinical diagnosis is highly suggestive.
Pain is frequently relieved with complete excision. Following an incomplete resection, recurrence is common.
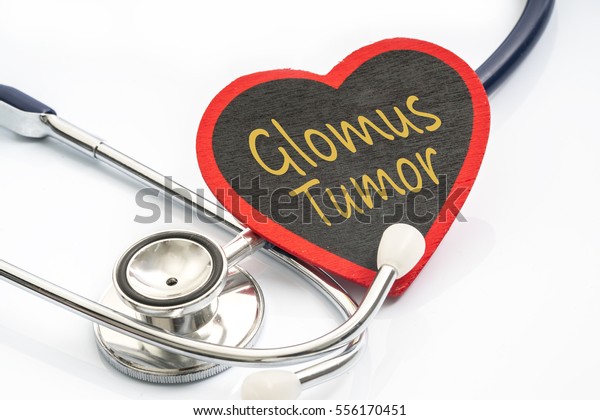
Detection of glomus tumors
Glomus tumors are benign tumors of the glomus body, a thermoregulatory conduit in the digits that cause pain. Glomus tumors of the fingers and toes are linked to the neurofibromatosis type 1 (NF1) monogenic condition and have only lately been recognized as part of the NF1 phenotype.
Results and Methods
We present the results of a multi-institutional study involving 15 people with NF1 and glomus tumors of the fingers or toes. Most people had at least two symptoms from the typical triad of localized discomfort, intense paroxysmal pain, and cold sensitivity.
In most cases, the appearance of the nail, finger, or toe is normal. Women are more likely to be affected than men. Multi-focal tumors are a common occurrence. Although magnetic resonance imaging may be helpful in some cases, there is often a long wait in diagnosis.
Clinical suspicion is crucial to diagnosis. Surgical removal of the tumor can be curative. However, recurrence and metachronous tumors are prevalent. Three of our patients showed indications and symptoms of CRP syndrome.
Summary
Glomus tumors in NF1 are more common than previously thought, and NF1 patients with fingertip or toe pain should be asked about it.
Glomus Tumors Treatment Options
If you have a glomus tumor, your Aurora neurosurgery team will work with you to determine the best treatment option for you, including experts from the Aurora Neuroscience Innovation Institute (ANII). For glomus tumors, your team may propose a mix of therapies, such as surgery and radiation.
The Expanded End nasal Approach (EEA) is a minimally invasive treatment in which the tumor is removed through the nasal passages, resulting in no incisions, a shorter hospital stay, and a quicker recovery.
A glomus jugulare tumor can only be treated with surgery. A tumor may need to be removed even if it is small and not causing severe symptoms. The tumor will continue to develop slowly and cause more issues as it grows larger if it is not removed. Surgery can be performed in a variety of ways.
A glomus tumor was surgically removed from a fingertip. The tumor is a translucent oblate spheroid in the incision’s center, with a horizontal dimension of about 4 millimeters. The preferred treatment for benign glomus tumors is surgical removal.
1. Surgical Removal of the Entire Tumor
Traditional neurosurgical methods can be used to remove a glomus jugulare tumor entirely. Because there are so many nerves in the area, the procedure is challenging, but no other therapy is required if the tumor can be removed without harming any nerves.
2. Stereotactic Radiosurgery (SRS)
Stereotactic radiosurgery isn’t a pretty surgical procedure. It entails directing X-rays at the tumor to eradicate the aberrant tissue. This approach, unlike standard radiation therapy, is more targeted and less likely to destroy healthy tissue.
3. Radiation Therapy Surgery
Traditional surgery to remove the majority of the tumor is sometimes paired with follow-up radiotherapy. The radiation is directed at the tumor remnants that the surgeon was unable to eradicate physically.
4. Epidemiology
Glomus tumors occur at an unknown rate. Multiple variants are uncommon, accounting for fewer than 10% of all occurrences.
5. Sex
Females are more likely than males to develop solitary glomus tumors, particularly subungual lesions. Males are somewhat more likely than females to have several lesions.
6. Age
Adults are more likely than children to develop solitary glomus tumors. Multiple glomus tumours appear 11–15 years earlier than single lesions, with one-third of occurrences occurring in those under the age of 20. Congenital glomus tumors are uncommon; they resemble plagues and are classified as a subtype of multiple glomus tumors.
Display of a Case
Glomus tumors are an uncommon mesenchymal neoplasm that affects the toes and fingers’ subungual tissues. Glomus tumors account for around 2% of all benign soft tissue tumors.
Glomus tumors with extra digital appearances are incredibly uncommon; just around 1% of glomus tumors are seen on the head. Lips (54.2 per cent), hard palate, gingiva, tongue, and buccal mucosa are the most common sites for ■■■■ glomus tumors.
The lung, trachea, heart, uterus, and stomach have all been involved in a few cases. Depending on the proportion of glomus cells, blood vessels, and smooth muscle cells, glomus tumors can be classified as solid (75 per cent of cases), glomangiomas with a vascular predominance (20 per cent), or glomangiomyomas with smooth muscle cell predominance (5 per cent).
Glomus tumors in the dermis or subcutaneous tissues of the extremities often measure less than one centimeter in diameter. On the other hand, glomus tumors in the head and neck region are more extensive, measuring 1 to 1.5 cm on average.
1. Evidence
There is no evidence that the size of the tumor affects the prognosis of the patient. There have been a few reports of malignant glomus tumors. Glomangiosarcoma is a cancerous version of a glomus tumor. Head and neck cancers are pretty uncommon.
Spector et colleagues described a case of cerebral metastases from a glomangiosarcoma of the head and neck. A case of glomangiosarcoma spreading to the jaw from a distant site was documented by Kreutz et al.
Histopathological investigation is used to determine whether glomus tumors are malignant. Tumors that are larger than 2 cm in diameter, have a moderate-to-high nuclear grade, and have an unusual mitotic figure of more than 5 per 50 HPF (high-power field) are considered very suspicious for malignancy.
2. Features
Flop et al. proposed classification of glomus tumors with atypical features in 2001, based on an analysis of 52 cases of glomus tumors and combining the histological features.
Features are as follows:
-
Malignant glomus tumors (large size and deep location, marked atypia with mitotic activity, as glomangiosarcoma).
-
Symplastic glomus tumor (only nuclear atypia).
-
Glomus tumor of uncertain malignant potential (superficial location with (histological features of benign glomus tumor with diffuse growth).
3. Cause
The cause of glomus tumors is unknown; however, family glomus tumors were discovered to be autosomal dominant with partial ■■■■■■■■■■■. Yoo et al. described a case of submandibular and parotid double glomus tumors.
Sixty per cent of patients with multiple glomus tumors have a positive family history, indicating that this is an inherited condition. In 1943, the first case of an ■■■■ cavity glomus tumor was documented.
In a survey of the English-language literature, we found only 27 cases of benign glomus tumors with ■■■■ involvement (Table). Rajendran et al. published the first intraoral case of glomangiosarcoma in English literature: a 51-year-old man with a 27-mm tongue glomangiosarcoma.
| CASES | YEAR | AUTHOR | AGE | GENDER | LOCATION | SYMPTOMS | SIZE(MM) |
|---|---|---|---|---|---|---|---|
| 1 | 2004 | Rallis et al | 85 | Female | Upper lip(mucosa) | pain | 13 |
| 2 | 2008 | Ide et al | 57 | Male | Upper lip | unknown | unknown |
| 3 | 2010 | Derand et al | 11 | Female | Lower lip(vermilion) | no | 3 |
| 4 | 2018 | Zou et al | 24 | Male | The floor of the mouth | pain | 28 |
| 5 | 2019 | Current case | 62 | Male | Lower lip(mucosa) | No | 10 |
Subungual glomus tumors cause stabbing pain, cold intolerance, and discomfort in the fingertips, whereas labial glomus tumors are usually painless and slow-growing. Patients between the ages of 40 and 70 are most likely to develop glomus tumors.
In contrast to the subungual location, which is more common in females, data show that the average age of presentation for labial tumors is 48.7 years without a sex preference.
Other areas, on the other hand, have a gender-balanced population. Surgical removal of the tumor is the only way to treat it. Subungual tumors have a recurrence rate of 4 to 15%, but labial glomus tumors have insufficient data to predict recurrence rates.
Summary
When compared to subungual glomus tumors, labial glomus tumors present in a distinct way. Because of the differences in clinical presentation, doctors have difficulty distinguishing these tumors from other, less painful lip lesions. For well-circumscribed, no tender lesions in the ■■■■ cavity, glomus tumors should be considered. We hope that this publication will raise awareness of this uncommon condition among professionals.
Is There a Long-Term Prospect?
The sooner you have the tumor removed, the more likely you are to make a full recovery. It’s easier to remove a smaller, less extensive tumor, and there’s less chance of damaging other vital structures accidentally.
It will be more challenging to remove a tumor that has spread to blood vessels and nerves. Even though removing this sort of tumor is a complex treatment, most people are cured after one or more procedures. The tumor may come back in some circumstances, necessitating further surgery.
Frequently Asked Questions (FAQs)
People asked many questions about “Glomus Tumor” few of them were answered below:
1. What is a glomus tumor’s defining symptom?
Pain, soreness, and temperature sensitivity are common clinical symptoms of glomus tumors, and their presence aids in diagnosis. However, diagnosing them can be challenging due to the wide range of symptoms and nonspecific symptoms associated with glomus tumors.
2. What are the symptoms of a glomus tumor?
The middle and inner ear structures are involved in a glomus jugulare tumor, which is a tumor of the temporal bone in the skull. The ear, upper neck, base of the skull, and surrounding blood vessels and nerves may all be affected by this tumor.
3. Is it possible to get cancer from a glomus tumor?
Glomus tumors, also known as paragangliomas, emerge from glomus cells and are benign (noncancerous) yet locally invasive tumors.
4. Can a glomus tumor be felt?
Glomus Tumors appear as a tiny, hard, reddish-blue lump beneath the fingernail. These lesions are typically tiny, with a diameter of less than 7mm. They can be excruciatingly painful, are temperature sensitive, and palpable.
5. Is it uncomfortable to have a glomus tumor?
Glomus tumors are a type of subungual lesion that can be extremely painful. Following modest trauma, they cause localized throbbing or lancinating discomfort, cold sensitivity, and acute pain. The clinical diagnosis is highly suggestive, but histology confirms the diagnosis. Pain is frequently alleviated by complete excision.
6. What are the treatment options for a glomus tumor?
Complete surgical excision is the curative therapy of choice for symptomatic solitary glomus tumors to reduce the risk of pain recurrence. In some cases with solitary glomus tumors, laser and sclerotherapy have been reported to be beneficial; however, complete excision is the best treatment.
7. Is a glomus tumor sporadic?
These benign tumors develop from one of the glomus bodies beneath the skin. Women are more likely to develop these tumors, which account for about 1% of all hand tumors.
8. Is a glomus tumor prevalent?
A glomus tumor (also called as a “solitary glomus tumor,” “solid glomus tumor,” or “solid glomus tumor”) is an uncommon neoplasm that arises from the glomus body and is typically detected under the nail, on the fingertip, or in the foot. Soft tissue tumors make up less than 2% of all cancers.
9. Is it possible for a glomus tumor to spread to other parts of the body?
Glomangiosarcoma, or malignant glomus tumor, is a sporadic mesenchymal cancer that affects the visceral organs. These tumors rarely spread, despite having malignancy-like histology. When the condition spreads, though, it is generally fatal.
10. Is it inherited to get glomus tumors?
The majority of glomus jugulare tumors occur by chance in people with no family history of the disease.
11. Is a paraganglioma a glomus tumor?
Glomus tumors, also known as paragangliomas, are:
-
Slow-growing, benign tumors that develop in the carotid arteries (the major blood vessels in your neck).
-
The middle ear.
-
The area below the middle ear (jugular bulb).
-
Glomus tumors are usually benign, but they can cause considerable damage to other tissues when they expand.
12. What is a stomach glomus tumor, and what does it look like?
Gastric glomus tumors are submucosal tumors that lack particular clinical and endoscopic features and are frequently confused with gastrointestinal stromal tumors. Shortness of breath and a persistent cough was seen in a 62-year-old Caucasian female.
13. What does glomus do?
Glomus type I cells are secretory, sensory neurons that respond to hypoxia (low pO2), hypercapnia (high pCO2), or acidosis by releasing neurotransmitters (low pH). Dopamine, acetylcholine, and adenosine are examples of signals sent to the afferent nerve fibers of the sinus nerve.
14. What causes the pain in glomus tumors?
Excruciating paroxysmal pain, extreme point soreness, and cold sensitivity are the hallmark symptoms of a glomus tumor. The contraction of myofilaments in reaction to temperature changes, increasing intracapsular pressure, is thought to be the pain mechanism.
15. Is it painful to have a schwannoma?
Schwannomas usually do not cause symptoms until they are large enough to impinge on the nerves surrounding them. Pain in the area controlled by the damaged nerve may occur on occasion. A palpable lump beneath the skin is one of the other typical systems.
Conclusions
Periungual glomus tumors are diagnosed as tiny tumors with exaggerated symptoms when they present clinically. An MRI can help establish the optimal surgical technique by pinpointing the tumor’s location.
The first excision gives you the best chance of a cure that is both practical and appealing. As a result, thorough tumor removal, meticulous planning, and a bloodless excision are required.
Histology backs up the initial diagnosis. When the tumor is located in the center of the nail, it is usually required to remove the nail, but for lateral tumors, a creative approach allows the tumor to be removed without causing damage to the nail matrix or nail bed.
The functional and cosmetic outcomes, as well as the absence of pain, indicate surgical success. One year following surgery, the patient had fully recovered and was symptom-free.
Related Article
https://howtodiscuss.com/t/rat-tumor-removal-cost/95535
https://howtodiscuss.com/t/symptoms-and-diagnostic-methods-for-ovarian-cancer/30165
