The term “heart failure” may be frightening. Heart failure does not mean the heart has failed or stopped working. It only means the heart of a person does not pump as well as it should.
Heart failure is a major health problem in the United States. It has affected about 5.8 million Americans. About 550,000 new cases of heart failure occur each year. It is the leading cause of hospitalization in people older than 60.
Heart failure can affect the right or left side of the heart, or both at the same time. It can be either an acute (short-term) or chronic(ongoing) condition.
In acute heart failure, the symptoms appear suddenly but go away fairly quickly. This condition often occurs after a heart attack. It may also be a result of a problem with the heart valves that control the flow of blood in the heart.
In chronic heart failure, however, symptoms are continuous and don’t improve over time. The vast majority of heart failure cases are chronic.
Heart failure and aging
Although the risk of heart failure does not change as people get older, people are more likely to have heart failure when they are older.
Heart Failure and Women
Women have equal chances to develop heart failure as men, but there are some differences:
- Women are likely to develop heart failure later in life compared with men.
- Women have more chances to have heart failure caused by high blood pressure and have a normal EF stress test.
Summary
If a person has a heart condition, it is important for him and his doctor to know his EF. EF can help doctor determine the best course of treatment. Measuring EF also helps healthcare team check how well treatment is working.
Types of Heart Failure
Heart failure can occur in either the left or right side of the heart. It is also possible for both sides of heart to fail at the same time.
Heart failure is also classified as diastolic heart failure or systolic heart failure.
- Left-sided heart failure
The most common type of heart failure is left-sided heart failure.
The left ventricle of heart is located in the bottom left side of your heart. This area pumps oxygen-rich blood to the rest of
the body.
Left-sided heart failure occurs when the left ventricle does not pump efficiently. This prevents the body from getting enough oxygen-rich blood. The blood backs up into lungs instead, which causes shortness of breath and a buildup of fluid.
Summary
The lower left chamber of the heart (left ventricle) gets bigger (enlarges) and cannot squeeze (contract) hard enough to pump the right amount of oxygen-rich blood to the rest of the body.
- Right-sided heart failure
The right ventricle of heart is responsible for pumping blood to lungs to collect oxygen. Right-sided heart failure occurs when the right side of the heart can’t perform its job effectively. It is usually triggered by left-sided heart failure. The accumulation of blood in the lungs caused by left-sided heart failure makes the right ventricle work ■■■■■■. This can stress the right side of the heart and cause it to fail.
Right-sided heart failure may also occur as a result of other conditions, such as lung disease. Right-sided heart failure is marked by swelling of the lower extremities. This swelling is caused by fluid backup in the legs, feet, and abdomen.
Summary
Right ventricular heart failure occurs because RV fails to maintain enough blood flow through the pulmonary circulation to achieve adequate left ventricular filling.
- Diastolic heart failure
Diastolic heart failure occurs when the heart muscle becomes stiffer than normal. The stiffness, which is usually due to heart disease, means that the heart doesn’t fill with blood easily. This is known as diastolic dysfunction. It leads to a lack of blood flow to the rest of the organs in the body.
- Diastolic heart failure is more common in women than in men.
Summary
It means the lower left chamber of the heart (left ventricle) is not able to fill properly with blood during the diastolic phase
- Systolic heart failure
Systolic heart failure occurs when the muscle of heart loses its ability to contract. The contractions of the heart are necessary to pump oxygen-rich blood out to the body. This problem is known as systolic dysfunction, and it usually develops when heart is weak and enlarged.
Both diastolic and systolic heart failure can occur on the left or right sides of the heart. people may have either condition on both sides of the heart.
- Systolic heart failure is more common in men than in women.
Summary
It happens when the left ventricle of the heart can not contract completely.
Stages of Heart Failure
- Class I
This is the period when the people are more likely to get heart failure
Symptoms
people don’t experience any symptoms during typical physical activity.
Outlook
Heart Failure at this stage can be managed through lifestyle changes, heart medications, and monitoring.
- Class II
people are in this stage if they never had symptoms of heart failure but they are diagnosed with systolic left ventricular dysfunction, which means the left chamber of their heart doesn’t pump well.
Symptoms
People are likely comfortable at rest, but normal physical activity may cause fatigue, palpitations, and shortness of breath.
Overlook
Heart Failure at this stage can be managed through lifestyle changes, heart medications, and careful monitoring.
- Class III
People are in this phase if they have systolic heart failure along with symptoms.
Symptoms
People are likely comfortable at rest, but there is a noticeable limitation of physical activity. Even mild exercise may cause fatigue, palpitations, or shortness of breath.
Overlook
Treatment can be complicated. Talk with the doctor about what heart failure at this stage may mean for you.
- Class IV
People are in this phase if they have systolic heart failure and advanced symptoms after they get medical care.
Symptoms
People are likely unable to carry on any amount of physical activity without symptoms, which are present even at rest.
Overlook
There is no cure for Heart Failure at this stage, but there are still quality-of-life and palliative care options. You will want to discuss the potential benefits and risks of each with your doctor.
Summary
Heart Failure can be life-threatening. If you suspect you or someone near you has Heart Failure, seek immediate medical treatment.
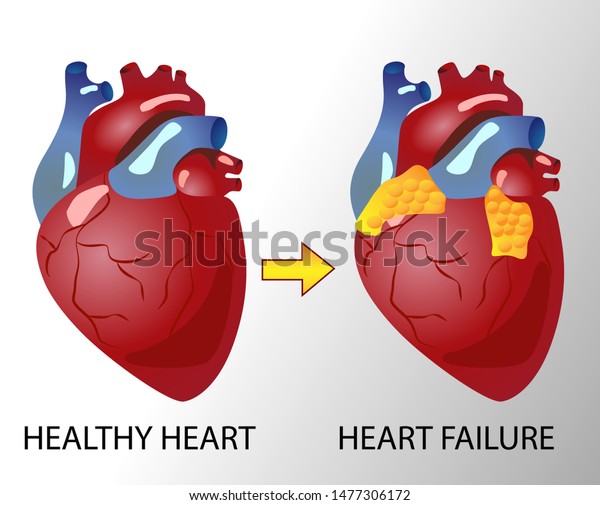
Causes of Heart Failure
Heart failure is most often related to another disease or illness. Heart failure can be caused by many medical conditions that damage the heart muscle. Common conditions are:
- Coronary artery disease (also called coronary atherosclerosis or “hardening of the arteries”). It affects the arteries that carry blood and oxygen to the heart (coronary arteries). The normal lining inside the arteries breaks down, the walls of the arteries become thick, and deposits of fat and plaque partially block the flow of blood. Over time, the arteries become very narrow or completely blocked, which causes a heart attack. The blockage keeps the heart from being able to pump enough blood to keep the organs and tissues (including heart) healthy. When arteries are blocked, people may have chest pain (angina) and other symptoms of heart disease.
- Heart attack A heart attack happens when a coronary artery suddenly becomes blocked and blood cannot flow to all areas of the heart muscle. The heart muscle becomes permanently damaged and muscle cells may die. Normal heart muscle cells may work ■■■■■■.
- Cardiomyopathy Cardiomyopathy is a term that describes damage to and enlargement of the heart muscle not caused by problems with the coronary arteries or blood flow. Cardiomyopathy can occur due to many causes, including viruses, alcohol or drug abuse, smoking, genetics and pregnancy (peripartum cardiomyopathy).
- Heart defects present at birth (congenital heart disease).
- Diabetes
- High blood pressure (hypertension). Blood pressure is the force of blood pushing against the walls of the blood vessels (arteries). If people have high blood pressure, it means the pressure in arteries is higher than normal. When blood pressure is high, heart has to pump ■■■■■■ to move blood to the body. This can cause the left ventricle to become thick or stiff. High blood pressure can also cause coronary arteries to become narrow and lead to coronary artery disease.
- Arrhythmia (abnormal heart rhythms, including atrial fibrillation).
- Kidney disease
- Obesity (being overweight).
- Tobacco and illicit drug use.
Other conditions that may increase the risk for developing heart failure include:
- an overactive or underactive thyroid
- heart valve disease
- emphysema, a disease of the lung
- severe forms of anemia
- ■■■
- AIDS
- certain cancer treatments, such as chemotherapy
Summary
The most common cause of heart failure is coronary artery disease CAD. Coronary artery disease is a disorder that causes narrowing of the arteries that supply blood and oxygen to the heart.
What are the symptoms of heart failure?
There may be times that symptoms are mild or may not have any symptoms at all. This does not mean that people no longer have heart failure. Symptoms of heart failure can range from mild to severe, and may come and go.
In general, heart failure gets worse over time. As it worsens, it may have more or different signs or symptoms. It is important to let the doctor know if you have new symptoms or if symptoms get worse.**
Common signs and symptoms of heart failure are:
- Shortness of breath or trouble breathing. You may have trouble breathing when you exercise, or when you rest or lie flat in bed. Shortness of breath happens when fluid backs up into the lungs (congestion) or when the body isn’t getting enough oxygen-rich blood. If people wake up suddenly at night to sit up and catch their breath, the problem is severe and they need medical treatment.**
- Feeling tired (fatigue) and leg weakness when you are active. When heart does not pump enough oxygen-rich blood to major organs and muscles, people become tired and their legs may feel weak.
- Swelling in ankles, legs and abdomen; weight gain. When kidneys don’t filter enough blood, body holds onto extra fluid and water. Extra fluid in the body causes swelling edema and weight gain.
- Need to urinate while resting at night. Gravity causes more blood flow to the kidneys when a person is lying down. So, a person’s kidneys make more urine and have the need to urinate.
- Dizziness, confusion, difficulty concentrating, fainting. People may have these symptoms because their heart is not pumping enough oxygen-rich blood to the brain.
- Rapid or irregular heartbeats palpitations When heart muscle does not pump with enough force, heart may beat faster to try to get enough oxygen-rich blood to major organs and muscles. People may also have an irregular heartbeat if heart is larger than normal (after a heart attack or due to abnormal levels of potassium in your blood).
- A dry, hacking cough. A cough caused by heart failure is more likely to happen when a person is lying flat and have extra fluid in the lungs.
- A full ( bloated ) or hard stomach, loss of appetite or upset stomach nausea
Summary
It is very important for everyone to manage other health conditions, such as diabetes, kidney disease, anemia, high blood pressure, thyroid disease and asthma or chronic lung disease. Some conditions have signs and symptoms that are similar to heart failure. If people have new or worsening non-urgent symptoms, tell healthcare provider.
Risk factors for heart failure?
Heart failure can happen to anyone. However, certain factors may increase risk of developing this condition.
People with diseases that damage the heart are also at an increased risk. These diseases include:
- anemia
- hyperthyroidism
- hypothyroidism
- emphysema
Certain behaviors can also increase risk of developing heart failure, including:
- smoking
- eating foods high in fat or cholesterol
- living a sedentary lifestyle
- being overweight
| chest X-ray | This test can provide images of the heart and the surrounding organs. |
|---|---|
| electrocardiogram | Usually done in a doctor’s office, this test measures the electrical activity of the heart. |
| heart MRI | An MRI produces images of the heart without the use of radiation. |
| nuclear scan | A very small dose of radioactive material is injected into the body to create images of the chambers of the heart. |
| catheterization or coronary angiogram | In this type of X-ray exam, the doctor inserts a catheter into blood vessel, usually in the groin or arm. They then guide it into the heart. This test can show how much blood is currently flowing through the heart. |
| stress exam | During a stress exam, an EKG machine monitors heart function while a person run on a treadmill or perform another type of exercise. |
| Holter monitoring | Electrode patches are placed on the chest and attached to a small machine called a Holter monitor for this test. The machine records the electrical activity of the heart for at least 24 to 48 hours. |
Diagnosis of Heart Failure
An echocardiogram is the most useful way to diagnose heart failure. It uses sound waves to create detailed pictures of the heart, which help the doctor evaluate the damage to heart and determine the underlying causes of the condition. The doctor may use an echocardiogram along with other tests.
Your doctor may also perform a physical exam to check for physical signs of heart failure. For example, leg swelling, an irregular heartbeat, and bulging neck veins may make a doctor suspect heart failure almost immediately.
How is heart failure treated?
It depends on the severity of the condition for treating heart failure. Early treatment can improve symptoms fairly quickly, but one should still get regular testing every three to six months. The main goal of treatment is to increase the lifespan.
Medication
Early stages of heart failure may be treated with medications to help relieve from symptoms and prevent condition from getting worse. Certain medications are prescribed to:
- improve heart’s ability to pump blood
- reduce blood clots
- reduce your heart rate, when necessary
- remove excess sodium and replenish potassium levels
- reduce cholesterol levels
Summary
Always speak with your doctor before taking new medications. Some medications are completely off-limits to people with heart failure.
Heart Surgery
Some people with heart failure will need surgery, such as coronary bypass surgery. During this surgery, surgeon will take a healthy piece of artery and attach it to the blocked coronary artery. This allows the blood to bypass the blocked, damaged artery and flow through the new one.
Doctor may also suggest an angioplasty. In this procedure, a catheter with a small balloon attached is inserted into the blocked or narrowed artery. Once the catheter reaches the damaged artery, surgeon inflates a balloon to open the artery. Surgeon may need to place a permanent stent, or wire mesh tube, into the blocked or narrowed artery. A stent permanently holds artery open and can help prevent further narrowing of the artery.
Other people with heart failure will need pacemakers to help control heart rhythms. These small devices are placed into the chest. They can slow your heart rate down when the heart is beating too quickly or increase heart rate if the heart is beating too slowly. Pacemakers are often used along with bypass surgery as well as medications.
Heart transplants are used in the final stages of heart failure, when all other treatments have failed. During a transplant, surgeon removes all or part of heart and replaces it with a healthy heart from a donor.
Prevention
A healthy lifestyle may help treat heart failure and prevent the condition from developing in the first place. Losing weight and exercising regularly can significantly decrease the risk of heart failure. Reducing the amount of salt in diet can also lower risk.
Other healthy lifestyle habits include:
- reducing alcohol intake
- quitting smoking
- avoiding foods high in fat
- getting an adequate amount of sleep
Summary
Early treatment is key in preventing the most serious cases of heart failure. Call the doctor right away if you are showing signs of heart failure or if you believe you have the condition.
Frequently asked questions
- How long can you live with heart failure?
Life expectancy with heart failure varies depending on the severity of the condition, genetics, age, and other factors. According to the Centers for Disease Control and Prevention (CDC), around one-half of all people diagnosed with heart failure will survive beyond five years.
- What are the signs of worsening heart failure?
Warning signs of worsening heart failure are:
-
Sudden weight gain (2–3 pounds in one day or 5 or more pounds in one week)
-
Extra swelling in the feet or ankles.
-
Swelling or pain in the abdomen.
-
Shortness of breath not related to exercise.
-
Discomfort or trouble breathing when lying flat.
-
Waking up short of breath.
-
Can heart failure be cured completely?
Currently, heart failure has no cure. However, treatment, such as medicines and lifestyle changes can help people who have the condition live longer and more active lives. Researchers continue to study new ways to treat heart failure and its complications.
Conclusion
Our treatment will depend on the type of heart failure we have and, in part, what caused it. Medications and lifestyle behaviors are part of every patient’s treatment plan. Our healthcare team will talk to us about the best treatment plan for us.
Related Articles

