Botox immunity or BOTOX tolerance occurs when a patient either generates antibodies against the botulinum or metabolizes the BOTOX medication incredibly quickly. As an outcome, the immune patient invests even more money on a treatment that simply does not work for her.

 Botox injections
Botox injections
Botox injections are the most frequently utilized nonsurgical cosmetic procedure on the planet. However, it does not work for everybody. Botox injections are rapid, comfortable, relatively inexpensive (when compared to surgery), and need no recovery. All of this, as well as the consequences.
There is a drawback, as with any medical procedure. Botox injections aren’t without risk, and the effects are transitory (three to four months is the norm). But what if Botox isn’t helpful for you?
Some individuals have had success with their first, second, or even third Botox treatments, only to discover that the effects are either considerably lessened or completely absent. Others seemed to be immune to Botox’s effects from the start.
 If Botox Isn’t Responding
If Botox Isn’t Responding
Some people can grow immune to the action of Botox, and it is a little true. It was formerly thought that the product didn’t operate since of incorrect storage or injector error, which included not employing the proper technique or dosing.
So because the patient’s antibodies were never brought into question, the standard approach at that point is to simply offer further shots. As a result, the immune patient pays even more money on a treatment that just does not operate for them.
Summary : Botox injections are quick, painless, affordable (when compared to surgery), and require minimal recovery time. Some people can indeed become immune to the action of Botox. Traditionally, it was believed that the product did not work due to incorrect storage or an injector’s error.
 Botox Resistance
Botox Resistance
These afflicted BOTOX injections have unsatisfactory outcomes, have a very short onset of treatment, or do not affect at all. True BOTOX tolerance is uncommon in company clinical studies, no more than 1.5 percent of people acquired “autoantibodies” to the treatment. Other experts say that just one out of every 10,000 individuals has true BOTOX resistance.
When BOTOX seems to be less effective for a patient, it is generally not due to actual BOTOX susceptibility.
 What the Botox Manufacturer Have to Say
What the Botox Manufacturer Have to Say
Since the growing popularity of Botox, researchers and doctors have found that resistance to Botox can build and that some people may be completely immune to its effect.
According to an Allergen spokesman, “occasionally some patients may develop an immunological response to BOTOX/BOTOX Cosmetics that may impair the effectiveness of the treatment.”
They point out that the protein complexes in their medication may cause neutralizing antibodies to be generated in some individuals. These antibodies, which are generated, by the immune system destroy Botox.
According to Allergen, this happens more commonly in those who receive frequent Botox injections or when administered in greater doses, such as when treatment cervical dystonia (although this is still a minor concern).
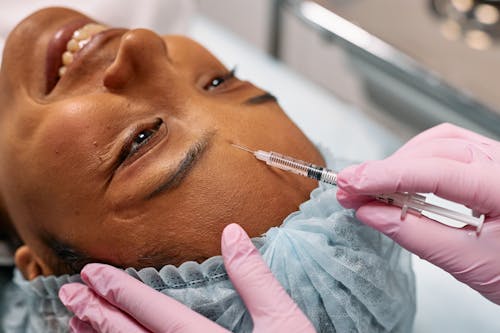
The label for Botox and Botox Cosmetic warns of the risk of an immune reaction. The label advises using the lowest effective dose and giving as much time between injections as feasible.
To put it simply, some patients develop Botox immunity. According to those who are aware of the problem of Botox resistance, the numbers are low 1%, and 3% of patients who are treated will acquire toxin-blocking antibodies.
These rates were reported in patients of patients receiving Botox therapy for cervical dystonia. Other studies of people who had cosmetics Botox found no evidence of an immune response.
There are also investigations being designed to assess how age and frequency of treatment may affect a person’s ability to develop Botox immunity.
Summary: True BOTOX immunity is uncommon in company medical tests, with only about 1.5 percent of persons acquiring “autoantibodies” to the therapy. According to some experts, just one out of every 10,000 people has actual Botox resistance. Botox and Botox Professional labels warn of the potential of an immune reaction. The label recommends using the lowest effective dose and separating injections more than feasible.
 Botox therapy and Immune system
Botox therapy and Immune system
Botulinum toxin type A is a polypeptide that can cause certain individuals’ immune systems to react by generating innate immunity, reducing the toxin’s potency.
Prior studies on this phenomenon focused on a single neurologic condition or on people who initially reacted angrily to Botox treatment but became less effective with subsequent sessions.
 Antibodies are needed
Antibodies are needed
The researchers recruited 596 people who had four botulinum shots over a year from 2013 to 2014 to determine the prevalence of autoantibodies in patients who got botulinum toxin injection for several neurologic conditions.
Patients were divided into subgroups based on their disorder: There had been 408 people with cervical dystonia, 47 persons with face hemi spasm (involuntary muscle contraction on one side of the face), 54 individuals with blepharospasm (involuntary blink or spasm of the eyelids), 52 people with different kinds of dystonia, and 33 people with stiffness.
The researcher classified people into three treatment plots to see if dosing altered the development of neutralizing antibodies: 0 to 350 universal dose units (UDU), 351 to 700 UDU, and fewer than 700 UDU.
The investigators also took samples taken from the patients, that were then stored for up to a year to look for immune responses.
 Antibodies Tested Positive
Antibodies Tested Positive
Neutralizing antibody was identified in 83 of the 596 patients who tested positive. There have been 64 cases of cervical dystonia, three cases of blepharospasm, nine cases of other types of dystonia, and five cases of stiffness. These antibodies were not generated in individuals with facial hemi spasm.
Summary : Botulinum toxin type A is a peptide that can induce certain people’s immune systems to respond by creating an immune response, hence lowering the toxin’s efficacy. Scientists recruited 596 persons who received four Botox injections over a year, from 2013 to 2014, to investigate the incidence of autoantibodies in Botox users. The researchers divided the participants into three treatment groups to see if dosing impacted the formation of autoantibodies.
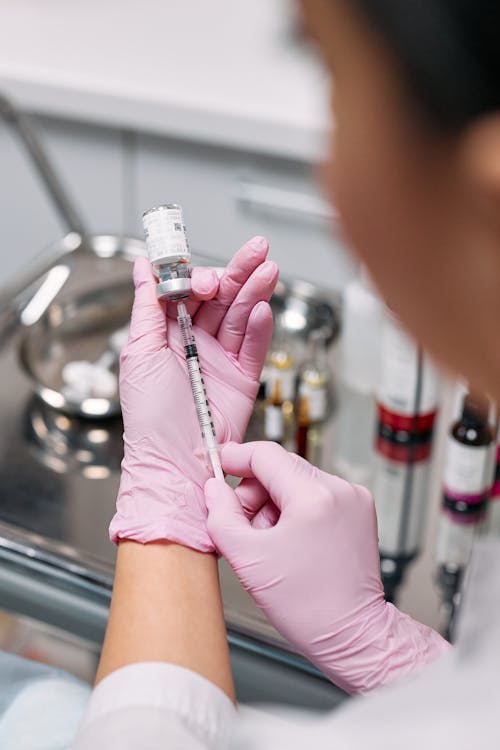
 Affect of Botox on the immune system
Affect of Botox on the immune system
Autoimmune Disease
The lymph nodes under the arms became extremely inflamed shortly after the injection, to the point that sufferers shouted in anguish if they were touched.
As an adolescent with limited anatomy, it never occurred to someone that injecting a toxin into a lymph node-infested region was generally not a great idea. It’s not even sure people realized it was a toxin. But found it normal when physicians were ok with it.
At the same time, those who gradually grew a 3-inch-long, 1.5-inch-tall scar on one side of the chest, barely an inch from where It was injected. It came out that they had morphea, a type of scleroderma in which the body makes excessive collagen, leading to what seem to be thick shiny scars on the epidermis.
While We can’t claim for definite that the injections caused the autoimmune disease or were the only factor, if you spend some time on Botox sites, you’ll notice that several people have gotten autoimmune disorders or health difficulties shortly after injection, some far worse than own.
Some may think so, but Botox only lasts a few months (For hyperhidrosis treatment, they say the effects last 4-14 months). The truth would be that we don’t know whether or not poison is eliminated from the body, and that if it does irreparable damage while it’s in there, you’re then left with the harm.
Summary : Injecting a toxin into a lymph node-infested region was not a good idea in principle. Shortly after the injection, the lymphatic system under the arms became highly swollen. Those who gradually developed a 3-inch-long scar on one side of their chest, barely an inch from where it was injected, thought it was normal when doctors cleared of it.
 Recommended Botox doses and regions
Recommended Botox doses and regions
| Regions | Recommended dose |
|---|---|
| Neck or head Area | Complete Dosage |
| Frontal | 20 units (4 sites) |
| Temporal | 40 units (8 sites) |
| Occipital | 30 Units (6 sites) |
| Corrugators | 10 units (2Sites) |
| Cervical Muscle | 20 units (4 sites) |
| Trapezium | 30 units (6 sites) |
| Total Range | 150 units to 195 units 31 to 39 sites |
 Frequently Asked Questions (FAQs)
Frequently Asked Questions (FAQs)
Some important queries related to the topic are
1. Why do Botox injections lose their effectiveness?
Botox becomes less effective in the long run as the body develops sensitivity to it. According to a new study, Botox injections may only provide a temporary berm against the eventual tide of aging. A tiny number of patients who receive recurrent botulinum toxin injection for skin treatment have an immune reaction, with the body producing antibodies to fight the poison.
2. Is it possible to develop Botox Immunity?
True BOTOX resistance is unusual manufacturer clinical trials, no more than 1.5 percent of patients developed “neutralizing antibodies” to the drug. Other doctors believe that only one out of every 10,000 patients has true BOTOX tolerance.
3. Is there any long-term consequence of Botox?
Long-Term Implications
There may be face muscle spasms weakness, causing eyelids to droop and eyesight to become distorted. These side effects will go away if you stay to use it. Botox® shots, like many other beauty treatments, have bad impacts despite being FDA approved.
4. When does Botox become unproductive?
Botox has no age limit, but it should not be used for cosmetic reasons on people under the age of 18.
5. What occurs if you discontinue taking Botox?
Signals among your nerves and the face muscles are disrupted when you receive Botox injections. When you stop taking Botox, your muscles will return true to their pre-treatment state. Your muscles and skin, on the other side, do not make up for a lost time by speed up the processing time.
6. Is it true that Botox affects the immune system?
Botox Has the Potential to Trigger an Immune Response
Botulinum toxin type A is a protein complex that can cause some patients’ immune cells to respond by generating neutralizing antibodies, decreasing the toxin’s potency.
 Conclusion
Conclusion
Finishing the topic of Botox immunity where it was discussed that how its produced and what are the reasons or factors of its development.
Botulinum neurotoxin infusions are a valuable treatment modality for a variety of therapeutic indications as well as for facial rejuvenation in the aesthetic field.
Secondary sensitivity to botulinum toxin preparation after repeated injections is an ongoing concern because successful therapy necessitates repeated injections over a considerable length of time. We present five case reports in which neutralizing antibodies to botulinum toxin type A developed after anesthetic injection and caused a secondary relapse.
The research papers presented in the report demonstrate that neutralizing antibodies can occur even at low doses of botulinum toxin type A in use in aesthetic practice, possibly leading to secondary drug resistance.
All aesthetic managers should consider using a toxin with the least immunogenic capability and become familiar with optimal practices for reducing the likelihood of immune responses developing.
Read also 
How long does Botox last
Derma Rolling
Immunity
