What is Heart failure?
Heart failure is a situation in which muscles are not able to pump blood towards the different parts of body to meet the body needs. What is heart failure? Heart failure a chronic condition and body is not able to receive proper blood supply and also the supply of oxygen is disturbed in this kind of situation. Heart failure does not mean that heart is completely lost or it will not work again, its just a disturbance in the working of the heart. When arteries of your heart become narrow and restricts blood supply then it leads to heart failure.
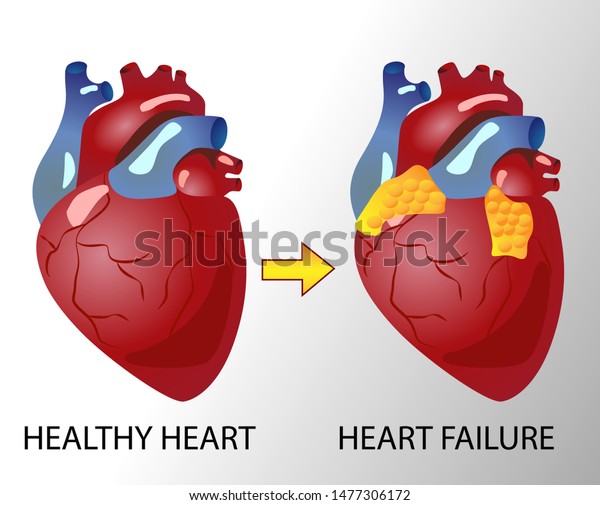
What is the cause of heart failure?
Heart failure can be due to many reasons and other diseases of the body can lead to heart failure. But there are some common causes which lead to heart failure. These common causes are High blood pressure, Coronary artery diseaseand Diabetes.
These are the leading and common causes of heart failure. These disease are found mostly in aged people and people having ages above 65 years are victims of these diseases and are on risk of heart failure. According to WHO, people having more weight than their age are more easy to fall prey to heart failure. on the other hand, Men in the world have high heart failure rate than women.

What are the 4 stages of heart failure?
As we know, heart failure is a long-term disease which is sometime normal and sometimes it gets worse. It can be of chronic situation. That’s why there are stages of heart failure to recognize intensity of failure. There are 4 stages of failure and they are;
-
Stage A - Stage A is considered as pre-heart failure. IN this stage, you are at risk of developing heart failure because you have some issues like Hypertension, alcohol addiction, diabetes, metabolism syndromes because these leads to heart issues. Pre- heart failure can also be due to heart problem history of the family.
-
Stage B - In this stage, patient is diagnosed with left systolic ventricular dysfunction. It is also referred as pre-heart failure because patients have no symptoms of heart failure. In this case, patients have echocardiogram fraction of 40-45% or less.
-
Stage C - patients with C stage of heart failure have proper diagnosed heart issues and they have shown proper symptoms in the past or still having them. C stage failure patients have symptoms like shortness of breath, physical weakness and fatigue.
-
Stage D - This is the final stage of heart failure and cannot be cured with the treatment. Stage D patients have advanced symptoms and have no chances to get better. The only solution of this kind of heart failure is heart transplant and sometimes heart surgery. This stage is chronic stage of failure.
Can you recover from heart failure?
Heart failure does not mean that your heart is no more and has stopped because if heart stops then how will you live. So, heart failure is the less functioning or irregular performance of heart that can be cured when your heart muscles get well and your body’s other disease are cured. When your heart starts pumping blood regularly again then your muscles are performing, this issue can be subsided for sometime but it can appear again.
Treatment
The treatment of common heart failure are the heart therapies and exercises that cure patients and remove causes that are the reason of heart failure like hypertension and diabetes can be removed by proper exercises.
But if you are suffering with chronic heart attack, then you need proper medication and if medication is not curing your issue, then you have to do heart surgery and transplant.

Frequently Asked Questions
Some question are asked frequently by patients suffering this disease;
How long can you live with heart failure?
People having Congestive heart failures have life duration depend upon their severity of disease, age, and health factors. According to CDC, people suffering from congestive heart failures can live beyond five years. It depends on intensity of disease and treatment factor. Some people survive their whole life with heart problems.
What foods should be avoided with congestive heart failure?
Heart diseases have link with food what you eat. So, eating healthy food and avoiding junk foods are positive steps to maintain your heart. Avoid salty food, potato chips and other oily eatables and try to drink more and more water because water maintain blood circulation level.
Can you recover from heart failure?
Heart failure in start can be cureable and heart keeps on working. Heart failure doesn’t mean that your heart goes to prevent working. It is the situation in which cardiac muscle doesn’t pump enough blood to satisfy the requirements of your body. There’s no treatment for coronary failure . Damage to your cardiac muscle may improve but heart problems remain till your life.
Conclusion
What is heart failure? Heart failure is a serious disease which restricts the blood flow and blood pumping function. If you are feeling start heart problems, then there is need to cure them and to take proper medical checkup. Heart failure is not too much risky, but if you are having chronic heart failure then it may lead to death.